 It starts in medical school, regularly appears in your medical training, sneaks around nursing schools and is an impetus for discussions in the ICU: The great myths about Hemoglobin (Hb) and Hematocrit (Hct). These two haematological lab-parameters are part of our daily life at work and are mostly measured together... as a package. Some clinicians look at haemoglobin levels, others prefer hematocrit levels... but then there is always someone making a great deal of differentiating between the two parameters and making all sort of diagnostic conclusions. 'Hct is better to determine dilution of the patient' or 'Acute blood loss is better determined by Hb than Hct'... and so on. So here's the question: What actually is the difference between Hb and Hct? Do we need to measure both in clinical practice? What's the difference? Hemoglobin levels are mostly measured by automated machines designed to perform different tests in blood. Within the machine, the red blood cells are broken down to get the haemoglobin into a solution. The concentration of haemoglobin is then measured by spectrophotometry using the methemoglobin cyanide method. Hematocrit levels in contrast are actually calculated by an automated analyzer... It is actually not measured directly! The analyser multiplies the red blood cell count by their mean corpuscular volume. What is Fact? There simply is NO difference between Hemoglobin and Hematocrit by means of clinical information!
Conclusion
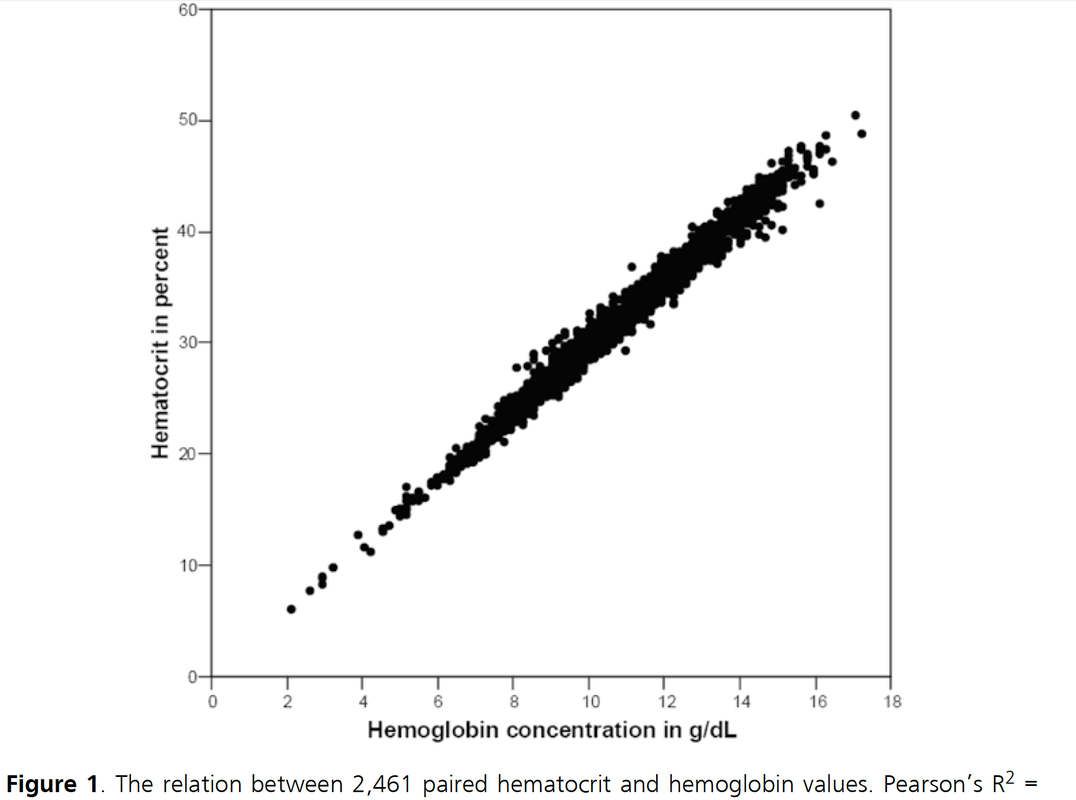
Once and for all! Nijboer J et al. J Trauma. 2007;62(5):1310-2.
Jonathan
27/8/2015 15:07:28
"The only rare exceptions are microcytic and polycystic anaemia" -- I don't know about polycystic anaemia, but microcytic anaemia isn't rare! 3/7/2017 18:02:47
Thank you I work in a lab we occasionally have to cancel and re-order blood work, I had a order for Hemoglobin and Hematocrit I decided to order only the hemoglobin and I begin to doubt myself as if I did the correct thing by ordering just the hemoglobin instead of ordering the two of them together as the doctor sent down to the lab.
Tim @BIJCorg
27/8/2015 15:39:40
Hi Jonathan,
Beth Neary
19/10/2016 17:13:05
thank you for this... I am an MD trying to explain this to a community group and this made it clear
Alicia
2/5/2017 15:48:22
Thank you for your post. Clinically, there is no need to measure both in most cases. However, can you confirm that for research purposes (estimating prevalence of anemia) if one clinic is collecting hematocrit and the other hgb, these clinics can't be compared regarding the level of anemia? I'm seeing Quinto, et al 2006 'Relationship between haemoglobin and hematocrit in the definition of anaemia' in Tropical Medicine and International Health, vol II (8). 1295-1302. The posted comments also suggest this is the case, right?. (I'm an MPH student in public health, so I apologize if this is a very novice question to ask....I'm a novice!).
Dear Alicia,
Paul
24/7/2017 04:43:38
So if they are the same the ratio Hct/Hgb should be constant ~ however mine has changed from 3.5:1 to 3:1 in the last two years. Obviously not the same !
pachchi
10/9/2017 09:13:47
Thanks for the post.!
Budding Doctor
6/3/2018 08:36:26
Really nice...Had this doubt for long time... you explained it clearly..
Mark Peters
11/3/2019 15:02:53
A correlation on a scatter plot is not proof of equivalence. For example if the gradient is not 1 then there will be a systematic difference. There is a close correlation between heart rate and respiratory rate but does not mean they contain the same information.
Simone
6/4/2019 11:25:15
Dear Timothy Comments are closed.
|
Search
|
||||||


 RSS Feed
RSS Feed


